Feminist approaches to global health policy have the potential to create more equal health systems. Considering and addressing power dynamics paves the way to tackle discrimination. More responsive health policies are expected to improve health for all.

Feminism and democracy are closely intertwined. Democratic principles, like representation, participation, accountability, human rights, and transparency, are equally core feminist values and enhance equality. Democracy entails diversity and accepting all people in their identities and intersectionalities. The same is true for feminism, which considers multiple approaches based on the different needs of people. Consequently, plural feminisms exist in contrast to one singular approach. Feminisms enable critical analyses of power and provide alternatives for a discrimination-free society. As such, feminist approaches to policy, in general, are essential for a more equitable future.
Why we need a system change: The role of power
Health inequalities cause harm and death every day. These inequalities arise from human-made health inequities that are avoidable and unfair. For instance, research confirms that racial discrimination leads to adverse mental health impacts, with depression being the most frequent outcome (Kluge et al., 2020; Paradies et al., 2015; Williams, 2018). Another example is the societal pressure caused by hegemonic masculinity and heteronormativity that increases suicidal ideation in men while it prevents them from seeking help (King et al., 2020). Such inequities are rooted in power regimes such as patriarchy, white supremacy, and capitalism. Inherent power asymmetries, often manifested through sexism, racism, and classism (among others) lead to adverse health outcomes for everyone, particularly for those who are oppressed in these systems, e.g. transgender people, Indigenous people, or (BIPoC) women.
The consequences are dire. For example, pre-term births in the US are 49 % more prevalent in Black women than non-Black women (March of Dimes, 2019). Global inequalities exacerbate the situation, with 94 % of maternal deaths occurring in low and lower-middle-income countries.
Racist and colonial attitudes are inherent in the global health system. Colonial continuities lead to a prioritisation of knowledge produced in the Global North while devaluing other forms of knowledge. This colonial legacy, which assumes the superiority of the Global North over the Global South, is still evident in global health today. For example, capitalist aspirations – merged with these racist and colonial attitudes - restricted access to Covid-19 vaccines for countries in the Global South. The pharmaceutical industry and supporting rich countries in the Global North chose profits over lives in times of a global crisis, inter alia by blocking a proposal to temporarily waive intellectual property rights at the World Trade Organization, which would have facilitated the global vaccine production and distribution. Neoliberal paradigms continue to shape the global health system, rendering health an unaffordable luxury for many. Similarly concerning is the gendered dimension of social inequities and its effect on health. Within the healthcare system, gender norms likewise persist. Although women comprise 70 % of the global health workforce, only 25 % of senior positions are occupied by female workers (WHO, 2019). In the private sphere, it is mostly women who engage in unpaid care work, increasing their risk for poverty and negative health impacts.
These inequities are structurally embedded and therefore avoidable and unjust. The concept of power is critical considering health inequities because its distribution in society determines privileges and oppressions. However, as the world is complex, multiple power regimes, e.g. patriarchy, ableism, and racism, exist and are interconnected. Intersectional approaches acknowledge this complexity and consider the synchronicity of different power structures in designing inclusive alternatives.
No progress on health without reproductive justice
What may seem like an abstract concept is best illustrated by the example of reproductive justice. The term was introduced by BIPoC women in the 1990s as resistance to dominant paradigms by white feminists. It combines aspects of reproductive rights and social justice (Ross & Solinger, 2017). Reproductive justice considers underlying power relations since focusing only on legal rights is not sufficient. Justice includes further (social) changes according to individual needs. Acknowledging intersectionality is central to reproductive justice because it recognises inherent power systems and the complexity of access to sexual and reproductive health. Reproductive justice demonstrates the intersection of gender, race, and class and further determinants as well as the significance of power, since political decisions on reproduction directly impact health. Historically, such policies have been influenced by capitalist and ideologist interests and used as an instrument to control (BIPoC) women’s bodies. The history of birth control and contraceptives roots back to slavery in the USA and is thus embedded in racism, classism, and sexism. Capitalist aspirations endorsed a high birth rate among enslaved Black women – more children meant more unpaid labourers. This changed with the end of slavery when eugenic ideology aimed for more white children. Hence, white women were denied terminating pregnancies while BIPoC women were forcibly sterilised. Poor women were also not supposed to have many children as they were regarded as inferior by society and thus a burden to the welfare state (Davis, 1981; hooks, 1982; Ross & Solinger, 2017).
Policies undermining access to reproductive healthcare point in the same direction today and provide the state with power over bodily autonomy and reproductive rights. The synergy of sexism, racism, and classism seriously restricts the realisation of reproductive justice. As this impacts the health and well-being of individuals, reproductive justice and health equality must be considered in tandem.
This demonstrates the necessity of intersectional approaches that are directed toward the political level. Because with the will to do so, political action can create changes that impact the whole society. By adopting the 17 Sustainable Development Goals, to be reached by 2030, the UN member states have already agreed to foster “Good health and well-being” (SDG 3), “Gender equality” (SDG 5), and “Reduced inequalities” (SDG 10). To ensure that this commitment is fulfilled, a feminist global health policy is needed.
But what exactly is meant by this?
Make global health policy more feminist
Globally, feminist approaches to policies have become increasingly prominent in recent years, most notably in foreign and development policy in the Global North. The application of feminist principles to global health policy – referred to as feminist global health policy (FGHP) – is in comparison still in its infancy, but distinct parallels can be drawn to more established feminist policy fields, as they are based on the same values and closely interlinked. Intersectoral exchange should be encouraged and coherent strategies across these policy fields promoted, to achieve global progress toward equality. A feminist approach to global health policy aims to truly realise the goals of health for all and equality. It is based on the understanding that negative health outcomes derive from oppressive structures and the dominance of hegemonic masculinity in patriarchy and intersecting systems. Evidence shows that the more equal a society is, the healthier it is. For example, Pickett and Wilkinson (2015) examined that income inequality is associated with worse health outcomes. Studies conducted in Europe confirmed that policies to enhance gender equality generate better health outcomes for all genders (Palència et al., 2017; WHO, 2018).
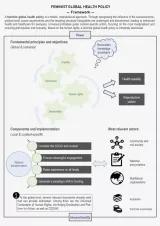
Just like feminist development policy, FGHP is centred on the concept of intersectionality and considerations of power and knowledge paradigms. By incorporating a feminist approach to global health policy, a human-centred, rights-based healthcare system free from discrimination is requested. The main objectives of this policy are the accomplishment of health equality and reproductive justice, to achieve better health and well-being for all. FGHP provides a nexus between the global and the local level, by entailing universal principles as well as recommendations and sensitivity for context-specific adaptations (see figure).
Fundamental, globally applicable values of human rights, equality, democracy, and decoloniality need to be incorporated. While adhering to these global principles, the implementation of a FGHP must be based on the respective needs at a local level. This includes sensitivity to the context, e.g. prevailing norms and beliefs, lifestyle habits, local healthcare systems, infrastructure, and geographic conditions. Accordingly, it is imperative to ensure meaningful engagement of the people concerned and to raise awareness at all levels. This renders the community as the most important actor. Accountability remains at the political level because policymakers are responsible for implementing a FGHP and creating an enabling environment. However, it is pivotal that policy processes are accompanied by civil society. Empowering people in the community to take on leadership roles allows for sensitive and meaningful change that is responsive to people's needs. This implies a radical transformation of the status quo – a demanding but necessary shift. Dominant knowledge paradigms persisting in global health, perpetuated by colonial continuities and power asymmetries, must be questioned and reconsidered. This includes for example the preference for standardised, quantitative indicators over lived experiences. To ensure financial feasibility and a departure from the current profit orientation fostered by the private sector, a shift to feminist funding principles is crucial. Besides community and policymakers, academia and feminist economists can function as secondary actors who help sustain a feminist approach to global health policy.
The discourse around FGHP is rather new. It is important to emphasise that there is no one universal solution. FGHP is characterised by its flexible adaptation for different settings. Therefore, policymakers and researchers are encouraged to consider the framework and to provide space for continuous discussions and reflection.
Feminist global health policy, in alignment with further feminist policy approaches, strives for a more just and equitable future. Current developments reveal that we are far from reaching that goal. Nevertheless, it is essential to not lose hope and to turn the vision into a lived experience one day. Because collectively, change is possible.
“It is in collectivities that we find reservoirs of hope and optimism.” (Angela Y. Davis)
References:
Davis, A. Y. (1981). Women, race and class. London: Penguin Books.
hooks, b. (1982). Ain't I a woman: Black women and feminism. London: Pluto Press
King, T. L., Shields, M., Sojo, V., Daraganova, G., Currier, D., O'Neil, A., King, K., & Milner, A. (2020). Expressions of masculinity and associations with suicidal ideation among young males. BMC Psychiatry, 20(1)
Kluge, U., Aichberger, M. C., Heinz, E., Udeogu-Gözalan, C., & Abdel-Fatah, D. (2020). Rassismus und psychische Gesundheit. Der Nervenarzt, 91(11), 1017–1024
March of Dimes (2019). 2019 March of Dimes Report Card. Healthy Moms. Strong Babies. Arlington: March of Dimes
Palència, L., Moortel, D. de, Artazcoz, L., Salvador-Piedrafita, M., Puig-Barrachina, V., Hagqvist, E., Pérez, G., Ruiz, M. E., Trujillo-Alemán, S., Vanroelen, C., Malmusi, D., & Borrell, C. (2017). Gender Policies and Gender Inequalities in Health in Europe: Results of the SOPHIE Project. International Journal of Health Services, 47(1), 61–82
Paradies, Y., Ben, J., Denson, N., Elias, A., Priest, N., Pieterse, A., Gupta, A., Kelaher, M., & Gee, G. (2015). Racism as a Determinant of Health: A Systematic Review and Meta- Analysis. PLOS ONE, 10(9), e0138511
Pickett, K. E., & Wilkinson, R. G. (2015). Income inequality and health: A causal review. Social Sciences & Medicines, 128, 316–326
Ross, L., & Solinger, R. (2017). Reproductive Justice: An Introduction. Berkeley: University of California Press
World Health Organization (WHO) (2019a). Delivered by women, led by men: A gender and equity analysis of the global health and social workforce. Geneva: World Health Organization
World Health Organization Regional Office for Europe (2018). The health and well-being of men in the WHO European Region: better health through a gender approach. Copenhagen: WHO Regional Office for Europe
Williams, D. R. (2018). Stress and the Mental Health of Populations of Color: Advancing Our Understanding of Race-related Stressors. Journal of Health and Social Behavior, 59(4), 466–485


